As Endometriosis Awareness Month comes to a close, and with 176 million women suffering from the condition worldwide, our feature aims not only to increase awareness of this mysterious condition in a biological sense, but also to share what it’s like for women who suffer with endometriosis in Malta, the women who live with crippling chronic pain in their every day lives. In addition, we’re highlighting the local support network for those who may be suffering alone and are looking for a community of like-minded women who know exactly what you are going through.
So, if you or someone close to you has endometriosis, or if you’d just like to know more about a widespread condition that has been kept mostly under wraps, let’s get learning!
The Science – with Dr. John Thake
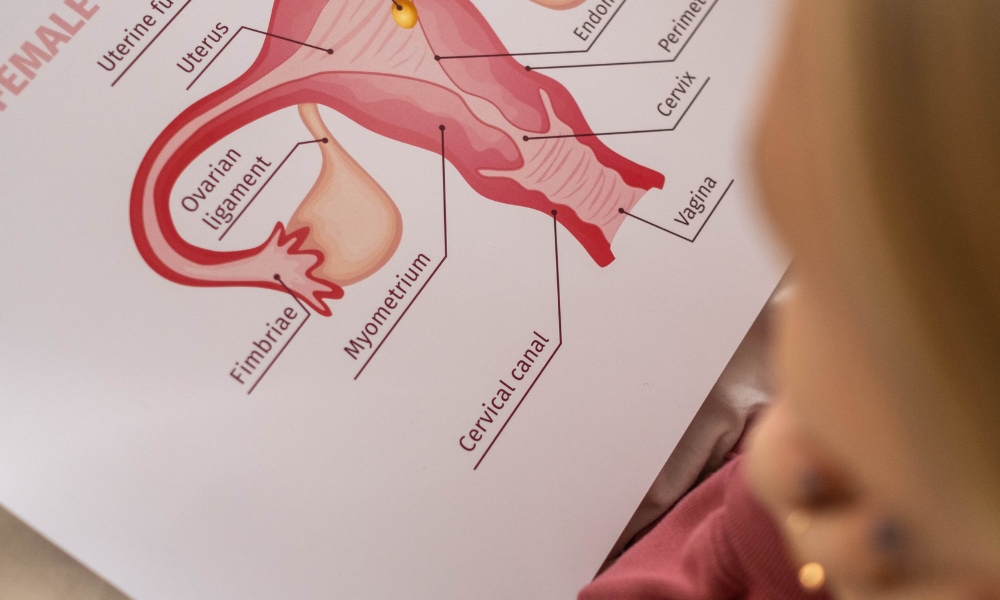
What is endometriosis?
Endometriosis is a medical condition which can cause severe disruption to a woman’s physical and psychological wellbeing.
It derives its name from the word “endometrium” which is the medical name for the inner lining of the uterus. Women who have endometriosis have these cells growing outside the uterus, usually in the pelvic area but rarely in other locations, as far flung as the brain or the lungs.
We’re not sure why or how this happens, but when endometriosis occurs, these cells (wherever they are) respond to hormonal changes in the same way that the lining of the uterus does, so when the woman menstruates, the endometriotic tissue will also bleed. This causes varying degrees of inflammation which can result in levels of adhesion formation (the body’s response to inflammation inside the tummy) and this tends to be the source of most of the symptoms and problems arising from endometriosis.
What are the symptoms?
Some women with endometriosis have no symptoms. Indeed the symptoms themselves may not necessarily be a good indicator of the severity of the underlying disease; some women with severe symptoms may have minimal disease and some women with severe disease may have minimal symptoms.
These include pain, which may occur before or during monthly periods, during or after sex, or when urinating or having a bowel movement (often during monthly periods).
Endometriosis may also be discovered incidentally when a couple are having trouble getting pregnant, or during a routine visit to the gynaecologist. For example, a growth on an ovary may be present which a doctor can feel during an internal examination or which can show up on an ultrasound of the pelvis. It is important to remember that these symptoms can also be associated with other conditions besides endometriosis.
Since there are no specific tests for endometriosis the diagnosis is usually a clinical one, obtained from the history and examination. And even though an ultrasound might help when there are endometriotic cysts (ovarian cysts filled with endometriotic tissue) of the ovaries, the only way to make a definitive diagnosis is by surgery.
This involves keyhole surgery (Laparoscopic Surgery), and may not only be diagnostic, but can also be interventional – when the surgeon may perform keyhole operations to remove cysts or adhesions, or burn off spots of endometriosis which could be the cause of the symptoms.
What are the treatment options?
The surgery mentioned above is one way in which endometriosis may be treated, but it can be tackled in different ways. We often opt for less invasive forms of medical treatment using various hormonal approaches, and this has to be tailored to the patient’s needs. These may include factors such as her desire to conceive (at the time of seeing the doctor or in the future), or the severity of the pain and its effect on the woman’s life. The management of any given patient will therefore depend on symptoms and on her fertility plans.
The doctor might use:
- Painkillers can be used to treat the pain caused by endometriosis, but it doesn’t treat the condition. They can help if the woman is trying to conceive.
- The Pill or the Intrauterine Contraceptive System, both of which can stop or slow down the progress of the disease and help alleviate the pain in women who are not trying to conceive.
- Injections to stop periods. These again are not for women who wish to have a baby but are effective in reducing the symptoms of endometriosis. They cannot be used long term and can give the symptoms of the menopause.
Sometimes when no other treatments work, doctors might suggest a hysterectomy, which means removing the uterus. Depending on the age of the patient and other possible factors, the doctor may also remove the ovaries and fallopian tubes. It is obviously not possible to get pregnant after your uterus is removed.
All these treatments are available in Malta at Mater Dei Hospital as well as in the private sector.
Contributed by John Thake MD FRCOG Consultant Obstetrician and Gynaecologist, Mater Dei Hospital.
The Struggle – by Chloe Fenech

Can you imagine how Sisyphus felt, forever rolling that boulder up the hill, never to reach the top? In many ways, this is how living with endometriosis feels.
You’re forever rolling boulders. You feel pain, so you try to push through it with exercise, only for your pain to get worse or put you in bed the next day, you try this or that painkiller, only next time you realise the dose isn’t working, you need something stronger. You need more.
Endometriosis is one of the most common gynaecological complaints, yet so few people (including women) have heard of it. So often, our pain is dismissed as “women’s problems” or “normal”. It was labelled as hysteria and worse as recently as 50 years ago. Today, we’re often misdiagnosed, sent home with Panadol or not diagnosed at all. We must be advocates for our own health.
Endometriosis is so much more than a painful period. For some, the pain is constant. And the pain isn’t limited to reproductive organs. You can experience pelvic pain, bladder and bowel problems, leg pain, sciatic pain, chronic lower back pain, even pain in your diaphragm.
We’re told that pregnancy is a cure, yet so many women with endometriosis struggle with infertility. The one thing that we’re told could help (some women do report less symptoms after giving birth, but many report worse symptoms) is often the one thing that is impossible. Intercourse can also be extremely painful, so the whole idea of getting pregnant to help this condition feels like a cruel joke.
Then, if you do get pregnant, eventually, whether naturally or with interventions like medications or IVF, what if the endometriosis causes you to miscarry? If you don’t miscarry, how will your body cope now that it’s working for two, carrying that extra load and pumping twice as much blood, and all those hormones? How will you cope with a natural birth? And after, when your period returns, will you be in too much pain to hold your baby? If your baby is a girl, will she have it later in her life? There’s that boulder, slipping down the hill again.
It isn’t all doom and gloom. Like anyone with this condition, I live for the good days, the pain-free days. I feel empowered when I do find the right doctor or surgeon, willing to listen and offer support, I found an incredible community of women with endometriosis in Malta where we can share our stories, swap pain relief tips and remedies. I had some respite from the condition, for one glorious year before it came thundering back. I tried to get pregnant and failed. Then, despite the battles, the surgeries, the relapses, failed fertility treatments and more, I had my son. And the boulder feels just that tiny bit lighter.
The Support – with Anita Portelli

Endometriosis carries a substantial socio-economic impact, with pain so severe that it can leave a woman unable to finish her education or maintain a career. It can also have a significant effect on her quality of life, relationships and ability to have children. Doctors have been puzzled over why incidents of endometriosis, which was considered relatively rare as recently as the 1980s, have been skyrocketing. As you can imagine, all of this can have a devastating effect on the sufferer and those around them.
If you or someone you know is experiencing the condition, our Facebook Group, Endo Support Group – MALTA, currently has over 350 members who know exactly what you are going through. The group was established to help women in Malta who suffer from endometrioses, as well as to support and educate those who have someone close to them with the condition.
The page is completely private and we publish weekly updates as well as group content where our members share their experiences with each other and offer tips on managing mental and physical pain. You can also contact the support group administrators, Anita and Jenny, directly if you’d prefer to discuss things away from the Facebook page.
Follow the page here: FB Endo Support Group – MALTA.
Or email Anita (Malta) or Jenny (Gozo) at: [email protected].
Anita Leeanna Portelli was born in London and moved to Malta in 1976 where she is now working as a Gestalt Psychotherapist. As well as running the Malta Endometriosis support group, she is also Vice President of the Malta Infertility Network. Anita has a special interest in Health Psychology and working with individuals and their families suffering with chronic pain. She believes that enabling clients to lift their emotional conditioning is one of the best ways to give them the freedom to meet their needs effectively. Living with Endometriosis and Adenomyosis herself, and having undergone several related surgeries in Malta and abroad, led Anita to take over the running of the Endo Support Group together with Jenny Hill, who is based in Gozo.
If you’d like to read more about living with endometriosis in Malta, check out Chloe Fenech’s 6 Things Women With Endometriosis Want You to Know.



